Varicose Veins and Chronic Venous Insufficiency
-
December 3, 2025
- Posted by: Nina Rand
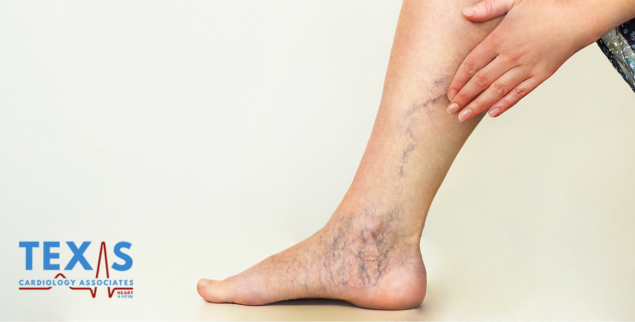
If you notice veins on your legs that appear raised, twisted, or achy by the end of the day, you’re not alone. These are often signs of varicose veins — one of the most common vein conditions in adults. In fact, about 25 million adults in the U.S. have them.
While they can be bothersome on their own, they can also point to a deeper issue known as chronic venous insufficiency (CVI).
Understanding the difference between the two (and how they’re connected) can help you take proactive steps to improve your comfort and protect your overall cardiovascular health.
What are varicose veins?
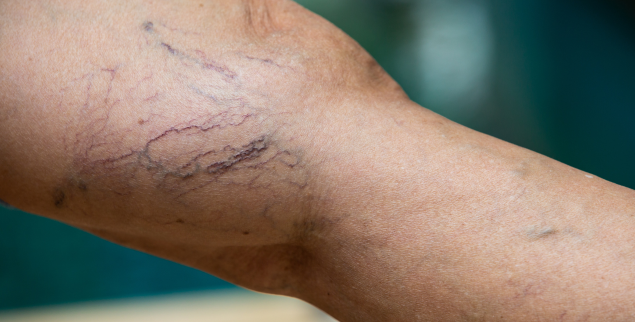
Varicose veins are enlarged, twisted veins that usually appear on the legs and feet. They occur when the tiny valves inside your veins (which help blood flow back up toward your heart) become weak or damaged. When these valves don’t close properly, blood can pool in the veins, causing them to stretch and bulge.
Varicose veins are very common, but they tend to affect more women than men and become more common with age. Pregnancy, standing for long periods, genetics, and even hormonal changes can all increase the risk for varicose veins.
What is the severity of varicose veins?
For many people, varicose veins are mostly a cosmetic concern. But for others, they can lead to aching, heaviness, swelling, or skin changes over time.
While varicose veins don’t always signal a serious condition, they can sometimes be a sign that your veins are struggling to circulate blood effectively. If that’s the case, you are likely experiencing chronic venous insufficiency.
What is chronic venous insufficiency?
CVI is a condition where the veins in your legs can’t efficiently return blood to your heart. This causes blood to pool in the lower legs, leading to swelling, skin discoloration, and, in more severe cases, sores or ulcers.
Who experiences chronic venous insufficiency?
AHA Journals states that 6 million American adults experience advanced venous diseases like CVI. It’s more common in people who have had varicose veins for many years, a history of leg swelling, or blood clots.
Can varicose veins cause chronic venous insufficiency?
Yes. Varicose veins and chronic venous insufficiency are closely related. Varicose veins are often an early warning sign of potential venous insufficiency because they start to develop when valves in your veins start to weaken.
If this problem becomes more widespread and affects the overall function of your veins, it can lead to CVI.
In other words, not everyone with varicose veins will develop CVI, but most people with CVI have a history of varicose veins.
What happens if chronic venous insufficiency goes untreated?
If left untreated, CVI can progress slowly and lead to greater discomfort, skin irritation, and even open wounds. With proper diagnosis and treatment, symptoms can be managed, circulation can improve, and further damage can often be prevented.
What are the differences between varicose veins and chronic venous insufficiency?
While varicose veins and CVI share some causes and risk factors, CVI is a more advanced stage of vein dysfunction. Recognizing early signs can help you seek treatment before symptoms progress.
Let’s take a look at an in-depth comparison between the two to help you better understand when to seek medical treatment.
CAUSES AND RISK FACTORS

Causes of Varicose Veins: Genetics, aging, pregnancy, prolonged standing or sitting, and hormonal changes can all contribute to weakened vein valves and the development of varicose veins.
Causes of CVI: While CVI can start with varicose veins, it can also result from prior blood clots, leg injuries, or long-term valve dysfunction that affects overall vein circulation.
Shared Risk Factors: Family history, age, gender (more common in women), obesity, and lifestyle factors that put strain on leg circulation can increase your chances of both conditions.
SYMPTOMS TO WATCH FOR
Varicose Veins: Typically, these veins are noticed first because they are visible and raised. Common symptoms include:
- Aching or throbbing in the legs
- Heaviness or fatigue by the end of the day
- Mild swelling around the ankles
CVI: Symptoms tend to be more persistent and may worsen over time. Look for:
- Chronic swelling in the lower legs
- Skin changes such as darkening, thickening, or itching
- Pain or discomfort that does not improve with rest
- Open sores or ulcers, in severe cases
DIAGNOSIS
Varicose Veins: Often diagnosed through a physical exam, sometimes with an ultrasound to check how the veins are functioning.
CVI: Requires more comprehensive vascular testing, usually an ultrasound or other imaging, to evaluate overall vein function and the extent of blood flow problems.
TREATMENT AND MANAGEMENT
Managing Varicose Veins:
- Lifestyle adjustments like regular exercise and leg elevation
- Compression stockings to improve circulation
- Minimally invasive procedures if veins are causing pain or worsening
Managing CVI:
- Compression therapy and lifestyle measures
- Medical management to address underlying vein issues
- Targeted procedures or interventions to improve circulation and prevent complications
When should I seek medical advice for varicose veins or chronic venous insufficiency?
It’s always a good idea to talk to a healthcare provider if you notice changes in your legs or veins. You should schedule an appointment with your cardiologist if you experience:
- Aching, heaviness, or pain that worsens by the end of the day
- Swelling in your ankles or lower legs
- Skin changes such as darkening, thickening, or itching
- Open sores or ulcers near the ankles
- Veins that appear suddenly larger, more painful, or inflamed
Even if your symptoms seem mild, early evaluation can prevent complications and help you feel more comfortable day-to-day.
A vascular specialist or vein care specialist can perform a simple ultrasound to check how your veins are functioning. From there, they’ll discuss personalized treatment options, ranging from lifestyle changes to minimally invasive procedures that can improve circulation and reduce symptoms.
If you’re currently noticing signs of vein issues or just want peace of mind, schedule a consultation with our team. Our specialists can assess your vein health and guide you toward the right next steps.
